Three reasons why Covid-19 challenge trials are so controversial
Would you deliberately infect yourself with coronavirus, if doing so would help get us all out of this mess more quickly? It sounds like the sort of hypothetical you might be asked in a philosophy lecture, but this week we learnt that the world’s first Covid-19 human challenge trial will be held in London from January.
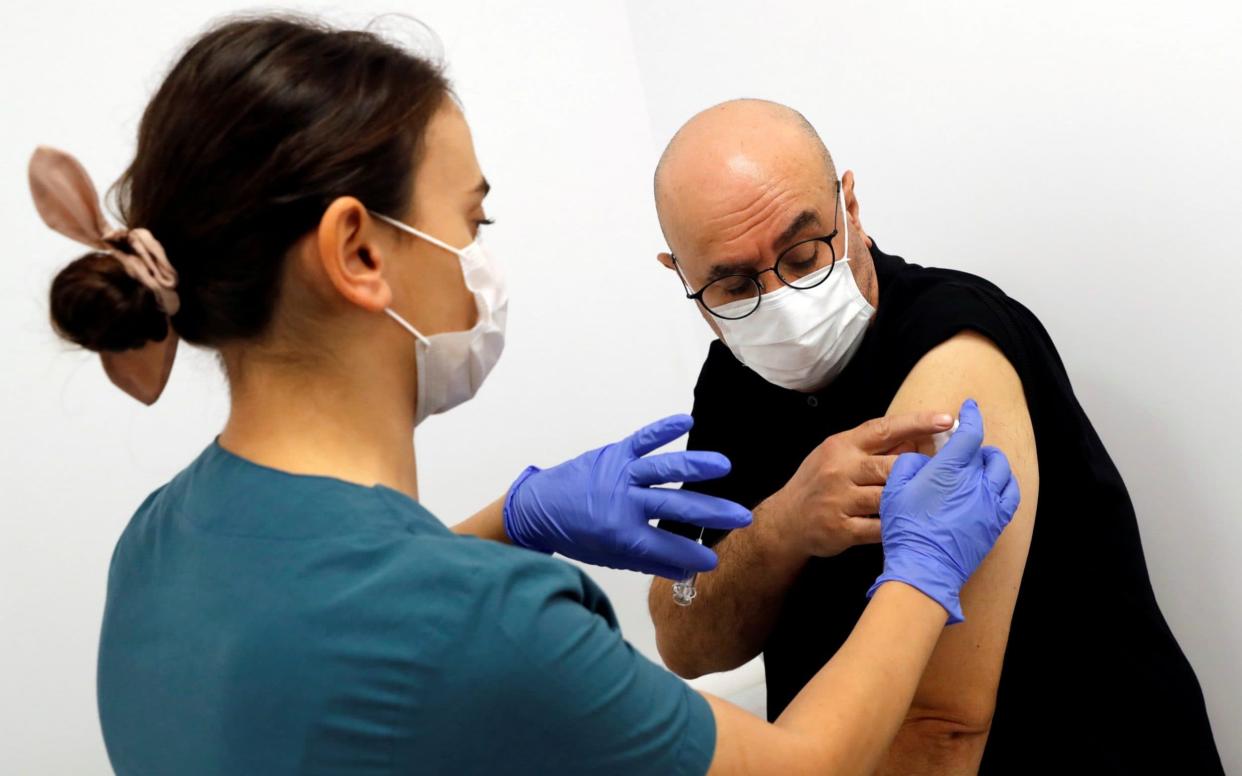
In a secure quarantine facility in east London, volunteers will be given a vaccine and then deliberately exposed to the Sars-Cov-2 virus.
Until now, the 80 or so Covid vaccine trials currently underway around the world have all followed broadly the same pattern: volunteers are given an injection and then told to live as normal, in the hope that enough of them become exposed to the virus in the course of their day-to-day lives to test whether it works.
But as cases have dwindled in many parts of the world, pressure has grown for authorities to allow challenge studies to quicken the process up.
More than 37,000 volunteers, 2,000 of whom live in the UK, have already pledged their willingness to participate through the 1DaySooner website. This includes a number of Nobel laureates and top ethicists, including Dominic Wilson, professor of medical ethics at Oxford University.
But challenge studies remain controversial. Why?
A chequered history
In the 18th century, English doctor Edward Jenner, known by many as the father of the vaccine, scraped cowpox particles into the skin of eight-year-old James Phipps, the son of his gardener, and then tried to infect him with smallpox. Thankfully, the boy survived, but the story is still used in medical ethics lectures as an example of exactly what not to do. More recently, in the 1940s, the US army stands accused of infecting thousands of psychiatric patients with malaria as part of its now-infamous ‘Malaria Project’; one in 10 died, according to the historian Karen Masterson.
Nowadays, even the mildest of clinical trials have to meet strict guidelines, and those experiments would never pass ethical muster. But the idea of deliberately exposing someone to a deadly pathogen is one that still makes some doctors uncomfortable. Prof Eleanor Riley, an immunologist at Edinburgh University, said this summer that challenge trials “should be incapable of causing severe illness in healthy individuals, or there should be a highly effective drug to clear the infection”.
She added: “None of these criteria are met for Covid-19, and I would be very concerned to hear challenge studies were being planned.”
There’s no cure
Challenge studies are already carried out in the UK for viruses like malaria, in which volunteers are placed in the vicinity of infected mosquitoes; as well as typhoid and tuberculosis. Meanwhile, the ‘Flu Camp’ facility in east London runs intermittent trials in which volunteers (often medical students) are infected with influenza or the common cold, and then observed in quarantine for up to two weeks, where they are treated to an en-suite bathroom and a PlayStation.
But the key difference is that those trials are very unlikely to kill one of their participants, and researchers usually have a “rescue remedy” on hand. Influenza and the common cold have a relatively mild effect on healthy young people (of the 2,300 young volunteers who have taken part in ‘Flu Camp’, nobody has died); and whilst malaria is deadly, it can be treated with the right drugs. In contrast, no cure yet exists for Covid-19, despite promising advances with remdesivir, which was originally developed to treat hepatitis C and was tried out against Ebola, and is now available for some coronavirus patients on the NHS.
A Covid challenge trial would effectively be testing a poison without an antidote. Prof Adrian Hill, director of Oxford’s University’s Jenner Institute and one of five researchers leading the Oxford vaccine trial – widely considered the world’s most promising vaccine candidate – has carried out challenge studies for malaria in the past, but stopped short of endorsing Covid challenge trials. “The difference with malaria is that we can always treat it,” he told the Telegraph in May. “We don’t do it for all infections – certainly, we don’t do it for HIV, which you can’t get rid of. Would it be ethical? And if you gave too much, how would you treat volunteers?”
The effects of Covid-19 on young adults are still unknown
Under mounting pressure to endorse challenge studies, the World Health Organisation (WHO) in May released a list of eight ethical hoops through which any trial would have to jump. Foremost among these was the rule that only healthy 18 to 30-year-olds should be allowed to take part.
This makes sense: the likelihood of a healthy twenty-something dying after contracting Covid is about one in 3,000, scientists say. This was the reasoning of 30-year-old Theo Sanderson, a geneticist at London's Crick Institute who told the Telegraph this summer that he would happily join a challenge study. “There's some level of risk, but we live with risk whenever we go skydiving, or whatever,” he explained. “And it's much less risk to me than it is to a 60-year-old doctor, say, who's going to work to protect his patients.”
But since then, we have learnt more about the virus, and particularly the effects of what some campaigners are calling “long Covid” – when symptoms linger on for months after the virus has left your system – which seems to affect younger adults more than we first thought.
This includes 27-year-old Charlie Russell, who spoke in the Guardian earlier this month about how, six months after contracting Covid-19, he still suffers from chest pains, migraines, breathlessness, dizziness, and exhaustion. “If I had known that I’d be this ill, I would have taken everything a lot more seriously back in March,” he said.

